Breast Health In The Time Of COVID-19: Volume 4
In this volume, I am completing my list of 19 steps to improve your breast health, during this COVID-19 pandemic. The first volume was about mammograms. In the second volume, I touched on alcohol, smoking, weight gain, hormones, sleep, and pregnancy. The third volume discussed exercise, vitamin D, the Mediterranean diet, pollutants, breast-feeding, and stress. Let’s finish up the list.
#13 Limit your fat intake.

#14 Decrease your consumption of caffeine from coffee, tea, and chocolate

#15 Vitamin E
For those of you who are having breast pain, consider a vitamin E supplement. The data is not strong, but there is very little downside to giving it a try. It is thought to be more likely to help those with cyclic breast pain, which is usually most severe in the week before menses. The typical dosage is 800 international units (IU) with meals. Dietary sources include olive oil, corn, soy, tomato, peanuts, spinach, almonds, and broccoli.
#16 Evening primrose oil (EPO)
One more option for those suffering with breast pain is evening primrose, a supplement you’ll find in most health food stores. As with vitamin E, the data is mixed, but there are a number of other purported benefits, so perhaps you can kill two birds with one stone. The typical recommended dosage is 1-3 grams daily.
#17 Be aware of your family history regarding cancer
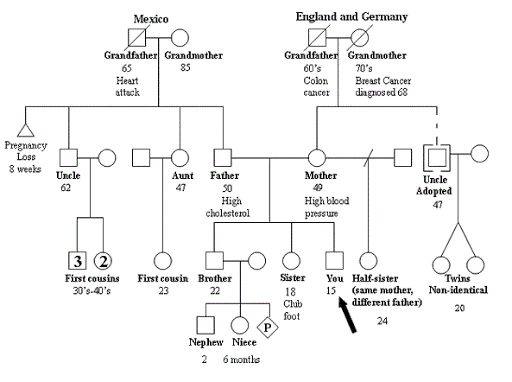
#18 Determine your individual risk for breast cancer
Your family history of breast or other cancers is one of many factors that can contribute to an increased risk for breast cancer. Once again, there are several sites available online to simplify calculation of one’s individual risk for breast cancer. Depending on your specific situation, one or the other may be more preferred. For someone with a lot of family members with breast or ovarian cancer, particularly at an early age, this calculator that is focusing on BRCA mutations might be preferred. The National Cancer Institute has a link that can be used as well. Here is a link to another one called Tyrer-Cusick, one that has a lot of popularity with breast specialists. It may be worthwhile to use more than one risk calculator and compare. They all have their quirks, and your calculated risk may differ from one to the other.
If you do a calculation for your breast cancer risk, be sure to record it, and share it with your primary care physician and any other specialist you might see regarding any breast problems.
#19 If your risk for breast cancer is increased, consider chemoprevention with tamoxifen or raloxifene.
If you are postmenopausal, and your breast cancer risk is high enough, you could decrease your risk by taking tamoxifen or raloxifene. If you are interested this option, discuss it with your primary care doctor, or ask for referral to a breast specialist. The recommended treatment continues daily for 5 years.
With the final volume, I’ll circle back to mammograms with some more detailed information. If you missed my first, second, and third volumes, these are the links. I’d love some feedback. Feel free to comment, and stay safe!

